Activity
Mon
Wed
Fri
Sun
Jun
Jul
Aug
Sep
Oct
Nov
Dec
Jan
Feb
Mar
Apr
What is this?
Less
More
Owned by Nisana
Vet-led community for backyard poultry keepers. Dr. Nisana, DVM, provides expert guidance on flock health, disease prevention, nutrition, & wellness.
Place for Veterinary Students to network while having access to material for clinics and the NAVLE. Scholarship and externship resource list.
Memberships
Skoolers
193.1k members • Free
Generational Revival
26.9k members • Free
Veterinary Scan - S - Kool
205 members • Free
Exotic Pet Education Platform
280 members • Free
Ranch Life - Goats & Alpacas!
20 members • Free
Exotic Pet Care
333 members • Free
Vetspan Collective
335 members • Free
Natural Pet Wellness Connect
58 members • Free
Dakoda Herbals Academy
24 members • Free
16 contributions to Pre-Vet Skool
🐟 Case Study: Why Are Koi Dying Overnight?
Meet Sakura, a prized 6-year-old koi in a backyard pond in California. Her owner calls in a panic on a warm September morning. Five of his twelve koi are dead and three more are lying on the bottom gasping. The water temperature is 73°F. You arrive and notice something immediately. The surviving fish are coated in thick excessive mucus and their eyes look sunken rather than bright. You check the gills on a freshly dead fish and find white and gray mottled patches where healthy red tissue should be. The owner mentions he added five new koi from an online seller three weeks ago without quarantine. This is Koi Herpesvirus. At 73°F, the temperature is perfect for viral replication. The gills are being destroyed faster than the fish can breathe. There is no antiviral treatment. Your first move is not medication but a PCR swab of gill and kidney tissue, followed immediately by a call to state animal health authorities. KHV is an OIE-listed reportable disease. The quarantine failure three weeks ago made this inevitable. 💡 The takeaway: In fish medicine, a four week quarantine is not optional. It is the difference between one sick fish and a pond full of dead ones. For the full course on this disease, see the classroom or follow the link below: https://www.skool.com/pre-vet-skool-9535/classroom/289939ea?md=ad951c90ea3b4b87909dc49e6936a6d2
0
0

🐴 Case Study: Why Is River Suddenly Refusing to Move?
Meet River, a 7-year-old Warmblood gelding on a Maryland farm sitting along the Potomac River. It is August. His owner calls because River has been feverish and off his feed for two days. Now he has developed profuse watery diarrhea overnight and this morning she noticed he is standing with his front legs stretched forward, refusing to walk. You check his digital pulses. Both forefeet are bounding and hot. River has Potomac horse fever, caused by Neorickettsia risticii, a bacterium he ingested weeks ago inside a mayfly that landed in his water bucket on a warm summer night. Now he is fighting diarrhea, endotoxemia, and developing laminitis simultaneously. You immediately start oxytetracycline 6.6 mg/kg IV in saline, administered slowly over 45 minutes. You pack his feet in ice. You add low dose flunixin to fight the endotoxin before it destroys his laminae. By morning his fever is gone. But the feet remain the battle. 💡 The takeaway: In Potomac horse fever, winning the infection is only half the fight. Save the feet. To learn more about this disease and case, the course is in the classroom or just follow this link https://www.skool.com/pre-vet-skool-9535/classroom/eada0165?md=7e3a779ffde345f6b24741ee37e028e2

0 likes • 2d
@Rosalie Kirkpatrick Love that you are already thinking about prevention, that is such a veterinary mindset! There is no mayfly spray unfortunately, but the prevention strategies are actually really interesting. The main approach is reducing what attracts aquatic insects to the barn in the first place, since mayflies and caddisflies are strongly drawn to bright lights at night during summer. Switching barn lights to yellow sodium vapor bulbs, moving lights away from water buckets and feed areas, and using insect screens on barn windows can all make a real difference. There is also a vaccine available for Potomac horse fever, though it does not completely prevent infection, it significantly reduces how severe the disease gets. So it is a combination of smarter barn lighting and vaccination that gives horses like River the best chance.
0 likes • 2d
@Rosalie Kirkpatrick Yes, caddisflies work the same way as mayflies in this disease. They are both aquatic insects that carry the same infected parasites inside their bodies, so a horse accidentally swallowing either one can get Potomac horse fever. And you are exactly right that they lay their eggs in water, which is why farms near rivers and streams see this disease most often in summer when these insects are emerging in huge numbers. As for the eggs themselves, they are not the dangerous stage. The risk comes from the adult insects that the horse accidentally swallows while drinking or eating near water. The Neorickettsia bacteria lives inside a parasite within the adult insect, not the egg.
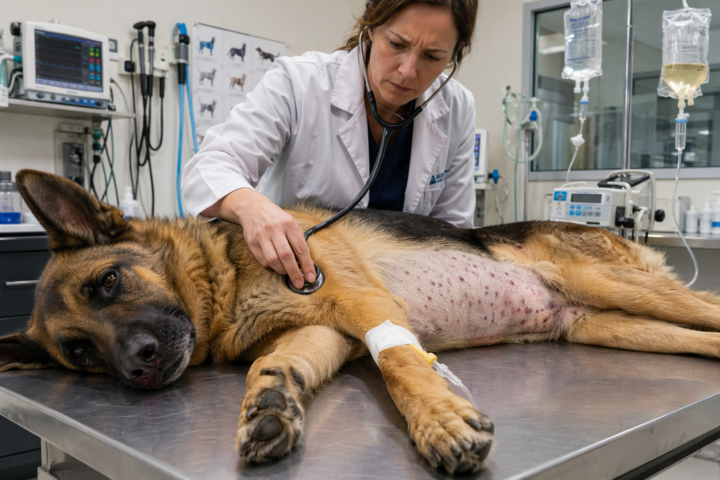
🐕 Case Study: Why Is Ranger Bleeding From His Nose?
Meet Ranger, a 4-year-old German Shepherd who comes in from rural Texas looking exhausted. His owner reports three days of fever, lost appetite, and now a nosebleed that will not stop. There are purple spots scattered across his belly. You notice his gums are pale and dotted with petechiae. Something is destroying his platelets. You run a CBC. Platelet count: 28,000 per microliter. Normal is above 200,000. You check the SNAP 4Dx test. Ehrlichia positive. This is canine monocytic ehrlichiosis, caused by Ehrlichia canis and transmitted by the brown dog tick, Rhipicephalus sanguineus. The bacteria invaded Ranger’s monocytes, triggering immune-mediated platelet destruction until his blood could barely clot. You start doxycycline immediately at 10 mg/kg twice daily for 28 days. Within 48 hours Ranger’s fever breaks and he is eager for food. German Shepherds like Ranger are especially vulnerable to the devastating chronic form of this disease. You caught this one early. 💡 The takeaway: Thrombocytopenia plus a dog from the South equals Ehrlichia until proven otherwise. For more information on this disease and other tick-borne diseases, head over to the classroom! https://www.skool.com/pre-vet-skool-9535/classroom/1f1964f8?md=9f4cee60096f4bd1abb8f3b0862d484a
0 likes • 2d
@Rosalie Kirkpatrick Such a great question and definitely not something most people have heard of before! Petechiae are tiny pinpoint red or purple spots that appear on the skin or mucous membranes like the gums. They happen when small blood vessels called capillaries break and leak a little blood just under the surface of the skin. In Ranger’s case his platelet count was so low that his blood could barely clot, so even the tiniest bit of pressure or normal wear and tear on his blood vessels caused these little spots to appear. Think of platelets like tiny plugs that seal leaks in your blood vessels. When Ehrlichia destroys them, those leaks have nothing to stop them.
0 likes • 2d
@Rosalie Kirkpatrick Great questions! Petechiae do not rupture when touched because the blood is already trapped under the skin, not in an open wound, so pressing on them does not cause additional bleeding or pain from the spots themselves. They do not hurt on their own either. The discomfort Ranger was feeling came more from the overall illness, the fever, and the weakness rather than the spots themselves. As for transport, the gentlest approach is a soft blanket lined carrier or the back seat of a car with minimal jostling, keeping him calm and supported. The most important thing is getting to the vet quickly rather than worrying too much about the spots themselves during transport
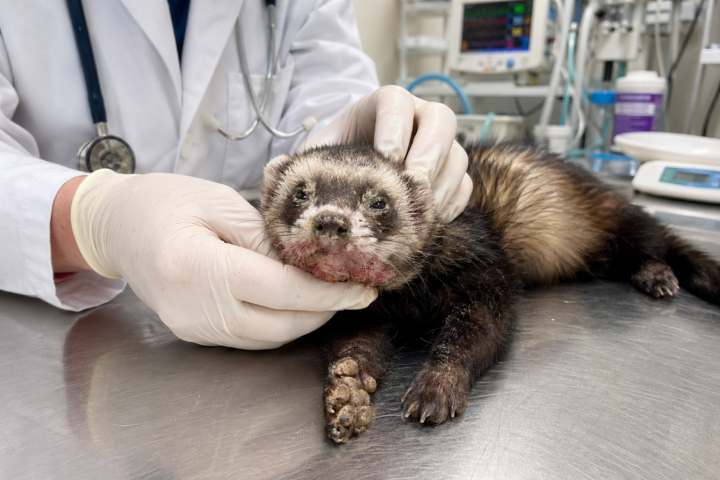
🐾 Case Study: Why Is Peanut’s Face Breaking Out?
Meet Peanut, a 10-month-old unvaccinated ferret whose owner noticed him scratching his face constantly two days ago. Today she brings him in because his chin is covered in a crusty red rash and his nose is crusted with thick yellowish discharge. You examine his feet. The footpads are thickening and roughening on both front paws. Your stomach drops. This combination, a facial rash plus footpad hyperkeratosis plus mucopurulent discharge in an unvaccinated ferret, is essentially pathognomonic for canine distemper virus. You ask about outdoor access. The owner mentions Peanut played in the backyard nine days ago. Raccoons visit that yard regularly. Nine days. Classic incubation period. You perform a conjunctival smear immediately, rolling the swab gently across the inner eyelid onto a glass slide. Under oil immersion you find what you feared: eosinophilic inclusion bodies inside the epithelial cells. You sit down with the owner. There is no cure. Nearly 100% of ferrets with CDV die. You discuss supportive care and prepare her for what comes next if neurological signs appear. 💡 The takeaway: In ferrets, vaccination is not optional. It is the difference between life and death. For a full course on this disease in ferrets see the classroom or follow this link: https://www.skool.com/pre-vet-skool-9535/classroom/f256bc88?md=233545f5a7b1454bb6f1056600ba512c
0
0
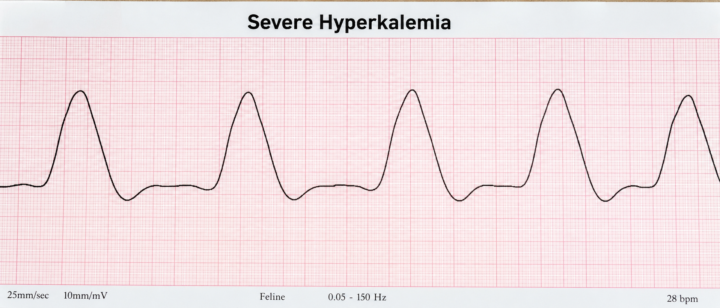
🐱 Case Study: Why Did Mochi Nearly Die Getting His Bladder Unblocked?
Meet Mochi, a 7-year-old male castrated Domestic Shorthair who comes in unable to urinate. His belly is rock hard and he can barely lift his head. Classic urethral obstruction. But when you hook him up to the ECG before sedation, something stops you cold. Heart rate: 28 beats per minute. No visible P waves anywhere on the strip. Wide bizarre QRS complexes developing a sinusoidal shape. You check his bloodwork immediately. Potassium: 9.4 mEq/L. Mochi’s obstructed bladder has been silently poisoning his heart for hours. The backed-up potassium has suppressed his sinoatrial node, wiped out his P waves, and is now pushing his heart toward ventricular fibrillation. You reach for calcium gluconate 10%, not the urinary catheter. The calcium does not lower his potassium but it immediately stabilizes his cardiac membrane, pulling him back from the edge. Then fluids, insulin with dextrose, and finally the catheter. Twenty minutes later his heart rate is 72 and P waves reappear on the strip. 💡 The takeaway: In a blocked cat, always check the ECG before reaching for the catheter. The heart may need saving first. For more information on this case, find the course in the classroom or follow this link below: https://www.skool.com/pre-vet-skool-9535/classroom/f78cd790?md=78613ab67ac849aaa7f8aa8e754fc504
0
0
1-10 of 16
@nisana-miller-8945
Bible believing wife to Shawn Miller, mom to Miriam, Owner of Praising Pastures, Covenantal Wings Veterinary Services, & Vet Skool Success Network
Active 23m ago
Joined Mar 30, 2026
INFJ
Heavener, Oklahoma

