
Write something
Why We Built This — And Why We Never Quit
What pushed us to build something different wasn’t a business idea. It was what we were seeing every day in the emergency department. A huge number of patients who come through the ER are there for one simple reason: they don’t have access to primary care. Not because they made poor decisions. Not because they didn’t care. Simply because access didn’t exist. Some arrive poorly treated—not from neglect, but from delay. Others wait four, five, sometimes six hours in an emergency department for minor illnesses that could have been handled safely and efficiently through telemedicine if access were available. That stayed with us. We weren’t trying to replace emergency medicine. We were trying to protect it—by keeping patients out of the ER when they didn’t need to be there, and by creating an economical, accessible way for people to get care earlier. From the beginning, we knew Direct Primary Care was the direction we wanted to go. But we also knew access alone wasn’t enough. Telemedicine had to be part of the solution. Not as a shortcut. Not as a replacement for real care. But as a way to remove unnecessary friction. We don’t believe doctors are “getting it wrong.” Most are overwhelmed—buried under red tape, documentation, and systems that make meaningful care harder every year. The intent is there. The time is not. At the same time, both of us were still working roughly 150 hours a month in the emergency department. We were very intentional about keeping those worlds separate. As tempting as it might have been from a business standpoint, we never pitched our clinic to patients in the ER. That line mattered to us. We wanted this built the right way—or not at all. There are plenty of colleagues who think we’re crazy for taking this path. That’s fine. What’s driven us hasn’t changed: an undying drive not just to be successful, but to create something better. Staying clinically grounded has always mattered. Emergency medicine keeps you honest. It also makes it clear that better access and longer appointments create space—for conversation, for prevention, and for alternatives before defaulting to the usual pharmaceutical path.
Community-Based Performance Medicine: A Strategic Outreach Model for DPC Practices
Most Direct Primary Care practices talk about prevention. Few operationalize it in a way that measurably improves outcomes while strengthening community trust. One highly effective strategy: Performance Medicine programs for high school athletes. This is not about supplements or selling services. This is about guiding developing athletes toward evidence-based optimization while protecting them from the rapidly growing black-market peptide ecosystem. The Problem Most Communities Don’t Realize Exists High school athletes are increasingly exposed to: - Social media-driven “optimization” messaging - Peer discussions about SARMs, peptides, and research chemicals - Influencers promoting unregulated compounds - Online vendors selling products labeled “not for human consumption” - Misunderstanding of legal vs illegal performance enhancement Many families assume their athletes are only using protein powder and creatine. That assumption is frequently incorrect. Without physician-led education, athletes often obtain: - Unverified peptides - Underground SARMs - Hormonal compounds - Contaminated supplements - Improper dosing protocols These introduce real risks: - Endocrine suppression - Fertility impact - Liver toxicity - Psychiatric effects - Impaired long-term athletic development Where DPC Has a Unique Strategic Advantage Direct Primary Care physicians have the flexibility to engage proactively in their communities without insurance constraints dictating care delivery models. Performance Medicine outreach allows practices to: - Establish early relationships with families - Provide objective, science-based guidance - Position the physician as the trusted authority - Create long-term continuity of care - Improve public health literacy This is preventive medicine in its purest form. What a Community-Based Athlete Optimization Initiative Can Include 1. Education First, Not Intervention First Host informational sessions for:
0
0

Social Media Sprint!
I hear from so many DPC docs that they hate social media. After a day full of caring for your family, patients, running your DPC, now it's 11pm and you're trying to figure out what to post on Instagram because you didn't get to it earlier. And honestly, sometimes you avoid posting because it's just not your thing, but you know it helps. That's exactly why the Social Media Sprint exists. It's a 14-day social media jumpstart beginning April 20th. Harmony Ops handles it all in one place: using a list of guided prompts, AI writes captions that sound like you, you approve them, and you post on up to 7 different social media platforms from one central page. Takes about 2-3 hours of setup and you'll have two weeks of posts scheduled & ready to go. You don't have to touch it after that. Plus your own branded "Is DPC Right for Me?" calculator page that educates prospective patients, crunches the numbers for them, and drives them straight to your door.When the sprint ends you keep the brand voice guide, posting planner, content guide, and all the posts to reuse anytime. $99. Cart closes April 18th. The only thing easier than this is paying someone else to do it entirely. And that costs a lot more than $99. https://reach.harmonyopshealth.com/sprint-home-page
1
0

Independent Practice Path - starts March 24
Many docs who are interested in Direct Primary Care spend a long time in the research phase. I call it "Procrasti-learning." Endlesslessly reading, listening to podcasts, joining groups, trying to figure out where to start, or waiting until everything is "perfect." (that never happens) Because I kept hearing the same questions from physicians who were considering opening a practice, I recently created a small physician cohort called Independent Practice Path. It’s an 8-week program focused on helping physicians move from thinking about opening a Direct Care practice to actively preparing to launch. We focus on things like: • mindset shifts involved in moving from employed physician to owner • learning how to explain the DPC model clearly • where and how to start conversations with potential patients • building early interest in the community • putting basic communication and nurture systems in place • collecting a waitlist of interested patients well before opening day The next cohort starts March 24. If anyone here is considering opening a DPC practice in the next 3-9 months and is curious about it, message me or go to the link here: https://ipp.harmonyopshealth.com/
0
0
Show patients the value of DPC
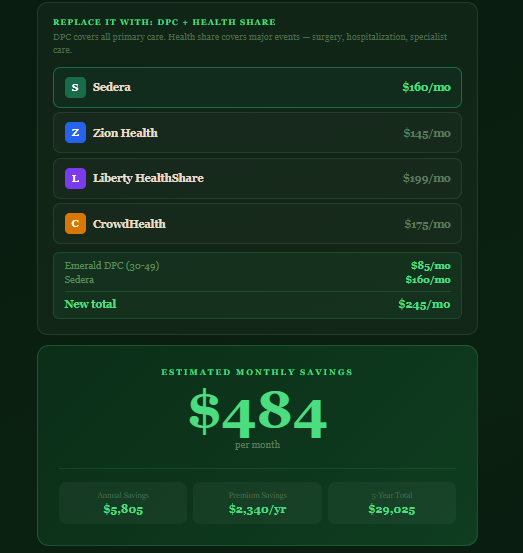
I built this app in 20 minutes--it's amazing what we can do now! The point of this is to show potential patients the amount of money that they could save with DPC combined with Health Share compared to insurance. Some people need to see it to believe it. https://24-7-bot.harmonyopsfordpc.com/savings
1-9 of 9

skool.com/firstcalldpc
Direct primary care gives unlimited access to your doctor, same-day visits, clear pricing, and no insurance—medicine built on trust.
Powered by



