Activity
Mon
Wed
Fri
Sun
May
Jun
Jul
Aug
Sep
Oct
Nov
Dec
Jan
Feb
Mar
Apr
What is this?
Less
More
Owned by Jonathan
Be ready when it matters. Real-world CPR, First Aid & Stop the Bleed training by a first responder, for families, schools, and first responders.
Memberships
Fit to Serve Cops
2.3k members • Free
Skill Prep
16 members • Free
Prepared Citizens
52 members • Free
Skoolers
194.3k members • Free
19 contributions to Not Today CPR and First Aid
“Slow Down”
In a stressful situation—whether it’s a medical emergency, a crisis at home, or you’re overwhelmed at work—sometimes the best thing you can do is slow down. This goes along with the idea of “Just Breathe.” Slow is smooth. Smooth is fast. When you’ve trained and prepared for certain events, your response often becomes second nature. You may think, “I know what to do. I’ve prepared for this.” That confidence can help you rise to the occasion and make a real difference. But it can also cause you to miss things. When you’re caught up in the heat of the moment, it’s easy to develop tunnel vision. You might overlook important details—like ongoing dangers in the environment, severe bleeding while focusing on compressions, or other critical problems happening at the same time. On the other hand, if you haven’t trained or prepared, you might freeze in the moment, unsure of where to start. That’s why it’s important to slow down and take a Tactical Pause. A tactical pause allows you to gather information, make better decisions, and maintain awareness throughout the entire event. Find a problem. Fix it. Pause. Reassess. Repeat. Taking just a few seconds to stop, breathe, observe, and think can give you the information you need to act effectively. That brief pause often leads to better outcomes than rushing in without fully understanding what’s happening around you. Sometimes the difference between chaos and control is just a moment to pause.
0
0

Just Breathe
Not as a cliché — as a survival skill. In high‑stress, traumatic situations, our bodies shift into overdrive. Breathing gets fast and shallow. Heart rate spikes. Fine motor skills drop. Brain fog creeps in. And if we don’t catch it early, we lose the clarity we need to actually help someone. This is where self‑awareness becomes a lifesaving tool. When you recognize, “My breathing is out of control,” you can take it back. A simple, intentional reset — deep breath in, deep breath out — can lower your heart rate, clear your head, and get you back in the game. It doesn’t take minutes. It doesn’t require training. It takes two seconds. A two‑count pause can shift you from panic to purpose. From scattered to focused. From overwhelmed to effective. When someone’s life is on the line, your ability to control your physiology is just as important as the skills you’ve learned. Slow your breath. Reset your mind. Then get to work.
1
0

Broken Bones, and what you need to know!
Framework: MARCH → then Secondary Injury Management 🩸 M — Massive Hemorrhage (FIRST, ALWAYS) Fractures love to bleed—especially femur, pelvis, open fractures. - Look for life-threatening bleeding - Apply: Tourniquet (high & tight if needed) Pressure dressing Wound packing if open + bleeding - Do not splint before bleeding is controlled 👉 Remember: A broken bone can kill via blood loss. 🫁 A / R — Airway & Respiration Usually intact with isolated fractures, but: - High-energy trauma = reassess - Rib fractures? Watch for: Shallow breathing Increasing pain Signs of pneumothorax 🩸 C — Circulation / Shock Fractures can cause internal bleeding. - Check: Skin (cool, pale, clammy) Mental status Radial pulse - Treat for shock: Lay flat (if safe) Keep warm Control pain if within scope 🧠 H — Hypothermia / Head Injury - Exposed patients lose heat fast - Use: Emergency blanket Jackets / vehicle heat - Head injury + fracture = higher priority 🦴 FRACTURE IDENTIFICATION Suspect a fracture if you see: - Deformity or unnatural angle - Swelling / bruising - Pain with movement - Loss of function - Bone visible = open fracture (medical emergency) ⚠️ If it looks broken, treat it as broken. 🔒 SPLINTING: THE GOLD STANDARD Rule: Immobilize the injury and the joints above and below Steps: 1. Expose the injury 2. Check CSM (Circulation, Sensation, Movement) 3. Realign only if needed to restore circulation (and trained to do so) 4. Pad generously 5. Splint & secure 6. Recheck CSM 🧠 Field-expedient splints: - Rifles (safe & unloaded) - Tourniquet windlass rods - Sticks / trekking poles - Cardboard / magazines - SAM splint = king 👑 🚫 WHAT NOT TO DO - ❌ Don’t ignore bleeding - ❌ Don’t force realignment unless circulation is compromised - ❌ Don’t leave jewelry on (swelling risk) - ❌ Don’t forget reassessment 🎯 SCENARIO (Think It Through) You respond to a vehicle vs pedestrian. Patient has: - Obvious lower leg deformity - Bleeding controlled with pressure - Complains of severe pain
1
0

Broken Bone Scenario – What Would You Do?
You’re at a school event or family gathering. Someone falls and has an obvious arm deformity. They’re in pain, bleeding lightly, and very anxious. 👉 What are the FIRST 3 things you would do while waiting for EMS? - Drop your answers below - There’s no judgment—this is how we learn - Read others’ responses and add what you’d do differently 💡 Being prepared isn’t about being perfect—it’s about acting instead of freezing.
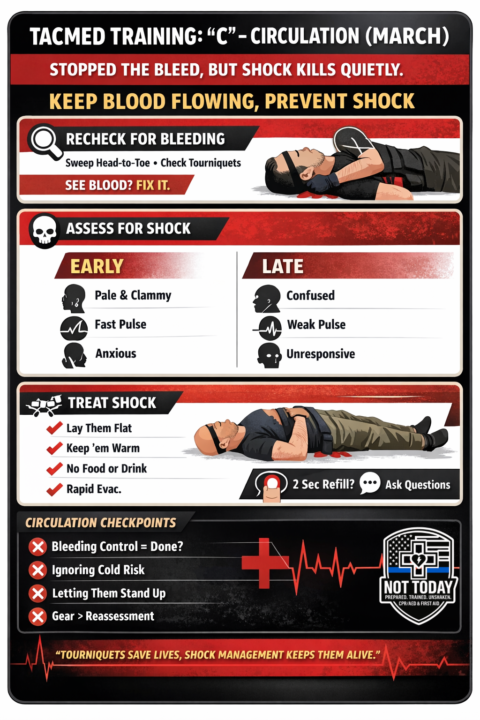
TACMED TRAINING: “C” – Circulation (MARCH)
Why “C” Matters You can stop the bleeding and manage airway/breathing—but if circulation fails, shock kills quietly. “C” is about keeping blood moving, organs perfused, and preventing preventable death. What “C” Covers (Plain Language) Circulation focuses on: - Identifying shock - Managing bleeding you may have missed - Supporting blood flow until higher care arrives Think: “Is blood moving where it needs to go?” Step-by-Step: Circulation Check 1️⃣ Recheck for Bleeding (You WILL miss things) - Quickly sweep head-to-toe - Look under clothing, behind legs, armpits, groin - Check tourniquets: Still tight? Bleeding stopped? Time noted? 👉 Rule: If you see blood, fix it before moving on. 2️⃣ Assess for Shock (This Is the Silent Killer) Early signs: - Pale, cool, clammy skin - Fast pulse - Anxiety, restlessness - Thirst Late signs (bad): - Confusion - Weak or absent pulse - Loss of consciousness 👉 You don’t need a BP cuff—use your eyes and hands. 3️⃣ Treat Shock (Simple, Effective Actions) - Lay them flat (if no contraindication) - Keep them warm (blanket, jacket, space blanket) - Control pain & anxiety (calm voice matters) - Do NOT give food or drink - Rapid evacuation / EMS activation 🧠 Cold + blood loss = clot failure. 4️⃣ Capillary Refill & Mental Status (Quick Field Checks) - Press fingernail → refill >2 seconds = poor perfusion - Ask simple questions: “What’s your name?” “Where are we?” “What happened?” Changes = worsening circulation. Common Mistakes to Avoid 🚫 - ❌ Assuming bleeding control = circulation handled - ❌ Ignoring temperature management - ❌ Letting patients sit or walk unnecessarily - ❌ Focusing on gear instead of reassessment Real-World Mindset Shift: Tourniquets save lives—but shock management keeps them alive long enough to matter. Circulation isn’t flashy. It’s discipline, reassessment, and calm control.
1
0
1-10 of 19
@jonathan-loser-2877
Community-focused CPR, AED & First Aid training led by law enforcement—equipping families and workplaces to respond with confidence.
Active 3d ago
Joined Jan 5, 2026
Azle, TX

