Activity
Mon
Wed
Fri
Sun
Jul
Aug
Sep
Oct
Nov
Dec
Jan
Feb
Mar
Apr
May
Jun
What is this?
Less
More
Owned by Adrian
Support for busy women who care for everyone else but lack the time for themselves—clear, quick guidance to finally prioritize your health.
Memberships
12 contributions to 24/7-OBGYN Health Coaching
How Unhealthy Relationships Affect Women’s Health (More Than You Think)
One thing that doesn’t get talked about enough in women’s health is how much stress from relationships can affect the body. In clinic, it often starts the same way. A patient comes in for something physical — irregular cycles, pelvic pain, fatigue, low libido, or trouble sleeping. We start talking about symptoms, and everything seems routine at first. But as the conversation continues, something else often comes up. She might pause and say something like: "Honestly… I’ve just been under a lot of stress lately." Then the story unfolds. Maybe there’s tension at home. Maybe there’s a relationship that feels emotionally draining. Maybe there’s constant conflict, lack of support, or the feeling of carrying everything alone. And what many people don’t realize is that the body doesn’t separate emotional stress from physical stress. When someone lives in a constant state of tension, the body can stay in stress mode. Cortisol rises, sleep suffers, hormones can become disrupted, and over time this can show up as: • Irregular menstrual cycles • Worsening PMS • Pelvic pain flares • Fatigue • Weight changes • Brain fog • Low libido Sometimes women come in thinking something is “wrong” with their body, when in reality their body is responding to the environment they’re living in. This doesn’t mean every symptom comes from stress. But it does mean our relationships, our emotional safety, and the amount of pressure we carry can have real physiological effects. One thing I often remind patients is this: Your body is not just reacting to what you eat or how much you exercise. It is also reacting to how safe, supported, and at peace you feel in your daily life. Health is not only physical. It’s emotional, relational, and environmental too. Sometimes the most powerful step toward healing isn’t another medication — it’s recognizing the sources of chronic stress in your life. Your health matters.
Hysterectomy or Not
Do you think that having a hysterectomy is always the best solution for fibroids and endometriosis issues. Or just a woman that has irregular periods.
0 likes • Mar 9
I believe each case should be evaluated individually based on a patient’s symptoms. For fibroids, if they are causing symptoms that significantly affect daily life, I would generally recommend treatment. However, if fibroids are found incidentally and the patient is not experiencing symptoms, I typically lean toward a more conservative approach. Endometriosis can be more complex, as pain may sometimes persist even after a hysterectomy.
Why High-Achieving Women Ignore Pelvic Pain — and How to Stop Normalizing It
Many high-achieving women say, “I almost didn’t come in—I kept telling myself it wasn’t that serious.” Not because they don’t care, but because they’re used to pushing through discomfort. When life is full, pelvic pain quietly becomes something you manage instead of something you question. Pain that causes you to plan your life around your cycle, rely on medication, avoid intimacy, skip workouts, or push through exhaustion isn’t something to normalize—even if you’re still functioning. These symptoms are common, but they are not normal. Pelvic pain is often the body’s early way of communicating hormonal imbalance, inflammation, pelvic floor tension, or conditions like fibroids or endometriosis. High-achieving women adapt well, but adaptation is not the same as health. A helpful shift is asking, “If this were happening to someone I love, would I tell her to ignore it?” That question alone raises your internal standard. What to Do Next If Pelvic Pain Is Affecting Your Daily Life If pelvic pain is interfering with your work, sleep, relationships, or ability to move through your day comfortably: 1. Stop minimizing it. Needing medication every cycle, avoiding intimacy, or planning your schedule around pain is enough reason to seek care. 2. Track patterns, not just pain. Notice when symptoms occur in your cycle, what makes them better or worse, and what else shows up—fatigue, bloating, mood changes, or bowel issues. 3. Start the conversation. Schedule an appointment with a women’s health provider. Telehealth counts. You don’t need severe symptoms to deserve evaluation. 4. Ask directly for answers. It's okay to ask, “What could be causing this?” and “What are my options?” Early clarity prevents long-term consequences. 5. Remember this:Your body isn’t interrupting your life—it’s offering feedback. Listening sooner protects your future health.

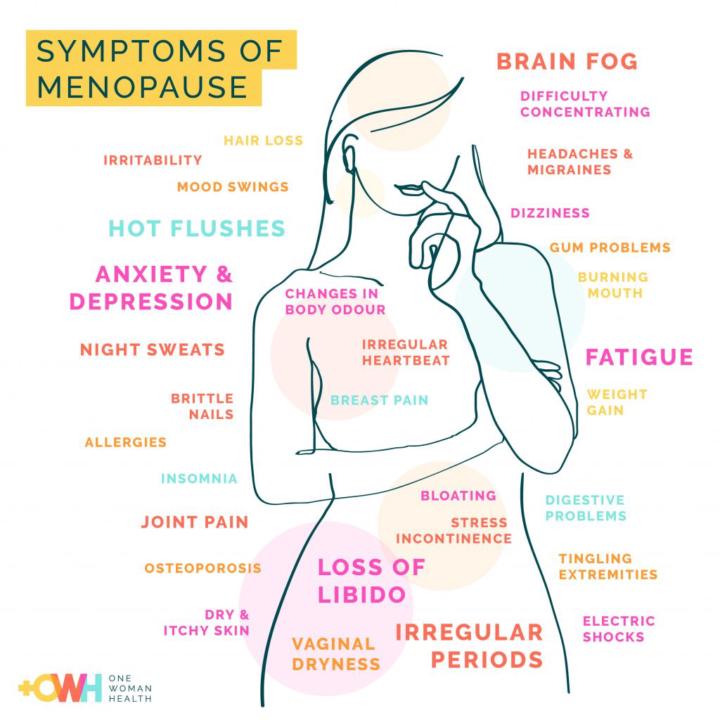
Menopause in African American Women: What’s Different, What’s Missed, and What Matters
Menopause is a universal transition, but the experience is not the same for everyone. For African American women, menopause often begins earlier, lasts longer, and can feel more intense — yet conversations around it are frequently delayed, minimized, or overlooked. Research consistently shows that African American women tend to experience hot flashes earlier and for a longer duration compared to other groups. These symptoms are often more disruptive, affecting sleep, mood, focus, and overall quality of life. When sleep is interrupted night after night, it doesn’t just cause fatigue — it can worsen stress hormones, increase weight gain, and heighten the risk of chronic conditions. Another important factor is that many African American women enter menopause already managing higher baseline stress. The cumulative effects of work demands, caregiving roles, systemic stressors, and health disparities can amplify menopausal symptoms. This isn’t a personal failure — it’s physiology responding to prolonged load. Menopause also intersects with conditions that disproportionately affect African American women, such as hypertension, diabetes, and cardiovascular disease. Hormonal shifts during menopause can increase insulin resistance, affect cholesterol levels, and influence where the body stores fat. When symptoms are brushed off as “just aging” or “something to push through,” opportunities for early intervention are missed. There is also a significant communication gap. Many African American women report feeling unheard when they bring up menopausal concerns, or they normalize symptoms because they were never taught what menopause could look like. Silence does not mean absence of symptoms — it often means lack of support. Menopause is not the end of vitality, strength, or purpose. It is a transition that deserves preparation, education, and individualized care. Understanding how stress, sleep, nutrition, movement, and hormone changes intersect empowers women to advocate for themselves and make informed choices.
0 likes • Jan 9
Thanks for sharing. What you’re describing is something many women notice during perimenopause, and for African American women it can start earlier and feel confusing at first. Irregular or skipped periods and those pregnancy-like symptoms can happen as hormones fluctuate. If it starts affecting how you feel day to day, it’s worth having a conversation with a provider. Thanks again for sharing that!
The Gynecologic Symptoms Women Ignore Because They’re Busy
Many women don’t ignore gynecologic symptoms because they don’t care — they ignore them because life is full. Work, family, responsibilities, and deadlines often come first, and symptoms get pushed to the background. Here are some of the most common symptoms: 1.) Heavy periods are one of the most common examples. Bleeding that lasts longer than usual, soaking through pads or tampons, or passing large clots often gets normalized as “just how my body is,” even though it can lead to anemia, fatigue, and brain fog. 2.)Pelvic pain is another symptom many women learn to live with. Pain during periods, intercourse, or throughout the month is often dismissed as stress, aging, or something to tolerate. But ongoing pelvic pain is not something you should have to power through. 3.)Irregular bleeding between periods or after sex is also frequently overlooked, especially when cycles are already unpredictable. Many women assume it’s hormonal or related to stress, but persistent changes deserve attention. 4.)Subtle symptoms matter too. Feeling constantly tired, short of breath, or mentally foggy may not feel “gynecologic,” but they can be signs of iron deficiency from heavy bleeding. Being busy doesn’t make symptoms less important. Your body doesn’t stop communicating just because your schedule is full. Noticing changes and getting checked isn’t overreacting — it’s being proactive. Here's a reflection questions I tend to ask all my busy patients and one that you should ask yourself: What symptom did you ignore the longest because life felt too busy to deal with it?
1-10 of 12
@adrian-simien-7609
OB-GYN dedicated to educating and empowering women with clear, compassionate, easy-to-understand health guidance.
Active 83d ago
Joined Nov 6, 2025


